Call to schedule your appointment!
Support your immune system with Vitamin D, Zinc, and Vitamin C. We offer a variety of supplement brands and can special order items for next-day delivery!
Are you considering changing your Medicare Drug plan for 2025?
Many plans may not be available in your area, please give us a call to schedule a Medicare Plan Comparison review to make sure you get the best plan for you!
Get Healthy!
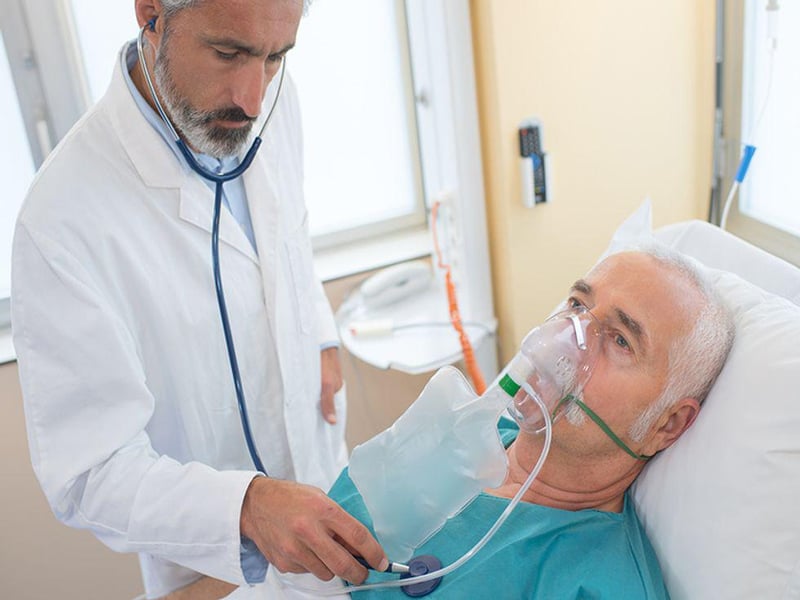
- Posted August 17, 2021
Dexamethasone Can Help the Sickest COVID Patients Survive. So Why Are Too Few Getting It?
There's strong evidence that the steroid drug dexamethasone can significantly lower hospitalized patients' risk of dying from COVID-19, but many who might benefit from it the most aren't getting it.
"Dexamethasone is a steroid that is used for the treatment of arthritis, inflammation and allergic reactions," explained Hemalkumar Mehta, who studied its use in treating COVID-19 patients. He said the drug can also combat the inflammation that can severely damage COVID-19 patients' lungs and other organs.
But in a new study, "approximately one out of five patients who may have benefited from dexamethasone did not receive it," said Mehta, who is assistant professor of epidemiology at Johns Hopkins Bloomberg School of Public Health, in Baltimore.
He and his colleagues pointed to a prior study conducted in June 2020. It showed that dexamethasone cut the risk of death by more than one-third in ventilated COVID-19 patients. It also lowered the risk by more than one-fifth among patients who'd been placed on supplemental oxygen.
However, after reviewing treatment of nearly 138,000 COVID-19 patients over 13 months, Mehta's team found that as many as 20% of patients who might be ideal candidates for the drug had not gotten it.
Treatment data was culled from a U.S. National Institutes of Health database of COVID-19 patients hospitalized at one of 43 U.S. health centers between Feb. 1, 2020, and Feb. 28, 2021.
During that time, 39% of patients were given dexamethasone. Older, white, male patients were more likely to be offered the medication, the findings showed.
Yet prescription patterns were more complex than they might appear at first glance.
For example, between February and May of 2020, only about 4% of hospitalized COVID-19 patients received the medication.
The numbers shifted dramatically starting in June 2020, with release of findings from the Randomized Evaluation of COVID-19 Therapy (RECOVERY) study. The shift suggests clinicians reacted quickly and positively to the new information.
Between June and July of last year, about one-third of hospitalized patients were already being given the drug. And by November, 53% were being offered dexamethasone treatment. By February 2021, that dipped to 33% of hospitalized COVID-19 patients.
Dexamethasone use rose to even higher levels among those COVID-19 patients on mechanical ventilators -- the group most likely to benefit from the therapy.
Among that group, between 78% and 84% were given either dexamethasone or a comparable type of (glucocorticoid) medication between July 2020 and February 2021, the study found. In other words, about a fifth of patients who may have benefited from dexamethasone weren't prescribed it.
Mehta said more research is needed to understand "reasons for potential underuse and what factors lead to inconsistent use among different health systems."
He cited several possible explanations, including a shortage of the drug itself, complex hospital protocols regarding medication administration, and poor quality of care at some facilities.
Other experts think the history of dexamethasone use should really be viewed as a glass half-full.
"The rapid incorporation of dexamethasone into standard of care -- at least in patients with COVID-19 on ventilators, as studied here -- literally within weeks of release of the clinical trials data is encouraging," said Dr. Marshall Glesby, associate chief of the division of infectious diseases at Weill Cornell Medicine in New York City, who co-authored an editorial that accompanied the findings.
Glesby suggested it's important, when analyzing dexamethasone use, to understand the context of a fast-moving pandemic characterized by a barrage of information and unsubstantiated claims.
For example, one drug -- hydroxychloroquine -- gained a lot of attention early on, after then-President Donald Trump touted its benefits, and the U.S. Food and Drug Administration gave it emergency authorization as a COVID-19 treatment.
But that authorization was ultimately revoked when subsequent research found the drug to be ineffective.
In contrast, dexamethasone took nearly the opposite trajectory, going under the radar at first, only to gain traction after solid research supported its use.
In that light, Glesby said, physicians on the front lines actually did pretty well separating the wheat from the chaff.
"Among the scores of potential therapies studied in clinical trials aimed at improving the treatment of COVID-19, dexamethasone was a home run," he noted. "It was shown to improve survival of hospitalized patients requiring oxygen."
And, Glesby added, its subsequent fast adoption and usage in the vast majority of patients who might stand to benefit is actually a "testament to how clinicians have been able to keep up with the avalanche of data, and do what's best for patients."
The study was published online Aug. 17 in the Annals of Internal Medicine.
More information
There's more about dexamethasone at the World Health Organization.
SOURCES: Hemalkumar Mehta, MS, PhD, assistant professor, epidemiology, Johns Hopkins Bloomberg School of Public Health, Baltimore; Marshall Glesby, MD, PhD, associate chief, division of infectious diseases, and professor, medicine and population health sciences, Weill Cornell Medicine, New York City; Annals of Internal Medicine, Aug. 17, 2021, online







